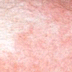
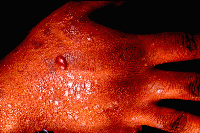
Dermatology
Diagnostic Approach
The arrangement of lesions may be distinctive. Grouping of tense vesicles is seen in herpes simplex and zoster. With herpes zoster, a linear arrangement is seen. Annularity (ring patterns) is typical in granuloma annulare, erythema multiforme, fixed-drug eruption, dermatophyte infections, some forms of Lyme disease, and secondary syphilis. Linear arrangement is seen in epidermal nevi, linear scleroderma, and contact dermatitis. In isomorphic reactions, lesions take the shape of the trauma to the skin (e.g., from scratching, rubbing, or other injury) as in psoriasis, lichen planus, and flat warts.
Special diagnostic approaches include:
1. Biopsy - important for histological diagnosis of obscure dermatoses.
2. Microscopic examination of scrapings - good for fungal infections.
3. Culture and antibacterial sensitivity testing - for acute bacterial skin infections.
4. Wood's light examination -examining the skin in a dark room under UV light filtered through Wood's glass ("black light").
5. Tzanck test - a smear of cellular material is scraped from the base and sides of a vesicle and stained with Wright's or Giemsa stain. Rapid and reliable test for diagnosing herpes simplex, herpes zoster, and pemphigus.
6. Viral cultures - if virus is suspected, vesicle fluid is put into a special transport media for culture at most medical centers.
7. Immunofluorescent tests - use of fluorescent microscopy to evaluate a patient's skin for in vivo antibody deposition. Good for SLE, discoid lupus erythematosis, pemphigus, dermatitis herpetiformis, , and pemphigoid.
8. Patch test - for allergic contact dermatitis.
9. Darkfield microscopic examination - for syphilis.
0. Hair counts - for alopecia.
Primary Skin Lesions
These are the first skin changes and are the best clues to diagnosis. They have not undergone changes yet.
Macules: flat, variably shaped discolored, and small (< 10 mm). A patch is a large macule (> 10 mm). Examples include freckles, flat moles, tattoos, port-wine stains, and the rashes of rickettsial infections, rubella, measles, and some allergic drug eruptions.
Papule: solid, elevated lesion usually <10 mm. A plaque is a plateau-like lesion >10 mm or a group of confluent papules. Examples include warts, some nevi, psoriasis, syphilitic chancre, lichen planus, some drug eruptions, insect bites, seborrheic and actinic keratosis, some lesions of acne, and skin cancers.
Nodule: palpable, solid lesion >5 or 10 mm which may or may not be elevated. Larger nodules (> 20 mm) are called tumors. Examples include keratinous cysts, small lipomas, fibromas, erythema nodosum, and some lymphomas and other neoplasms.
Vesicle: circumscribed, elevated lesion containing serous fluid that is < 5mm. A bulla (blister) is >5 mm. Examples are found with primary irritants, allergic contact dermatitis, physical trauma, sunburn, insect bites, or viral infections (herpes simplex, varicella, herpes zoster); other causes include drug eruptions, pemphigus, dermatitis, herpetiformis, erythema multiforme, epidermolysis bullosa, and pemphigoid.
Pustules: superficial, elevated lesions containing pus. They may result from infection or seropurulent evolution of vesicles or bullae. Some causes are impetigo, acne, folliculitis, furuncles, carbuncles, certain deep fungus infections, hidradenitis, suppurativa, kerion, pustular miliaria, and pustular psoriasis of the palms and soles.
Wheals (hives): transient, elevated lesions caused by localized edema. They are a common allergic reaction to such things as drugs, insect bites, heat, cold, pressure, or sunlight. Large localized areas of edema are called angioneurotic edema.
Purpura: general term to areas of extravasated blood. Petechiae are circumscribed punctate foci of extravasation. Large areas of extravasation are called echymoses. The term hematoma refers to an area of massive bleeding into the skin and underlying tissues.
Telangiectasia: dilated superficial blood vessels. They may occur in rosacea, certain systemic diseases (e.g., scleroderma) or in long term therapy with topical fluorinated corticosteroids. Most cases are idiopathic.
Secondary Skin Lesions
Secondary lesions result when primary lesions undergo a natural evolution (e.g., rupture of vesicle) or are manipulated by the patient (e.g., scratched vesicle).
Scales: heaped-up particles of horny epithelium. Common scaling rashes include psoriasis, seborrheic dermatitis, superficial fungal infections, tinea versicolor, pityriasis rosea, and chronic dermatitis.
Crusts (scabs): consist of dried serum, blood, or pus. Occurs in many inflammatory and infectious diseases.
Erosion: is focal loss of part or all of the epidermis. Often occurs with herpes viruses and pemphigus.
Ulcers: focal loss of the epidermis and at least part of the dermis. When ulcers result from physical trauma or acute bacterial infection, the cause is usually obvious. More obscure causes include chronic bacterial and fungal infections, various peripheral vascular diseases and neuropathies, systemic scleroderma, and tumors.
Excoriation: linear or hollowed-out crusted area caused by scratching, rubbing, or picking.
Lichenification: thickened skin area with accentuated skin markings.
Atrophy: paper-thing, wrinkled skin. Occurs in aged, discoid LE, after long-term use of topical potent corticosteroids, and sometimes after burns.
Scars: areas of fibrous tissue that replace normal skin after destruction of some of the dermis. May be caused by burns or cuts, and occasionally by diseases.
Principles of Topical Dermatology Therapy
Preparations:
- creams - most common; easy to apply
- ointments - stronger than creams; greasy; lubricates
- lotions - cool & dry inflammatory & exudative lesions
- solutions - convenient for scalp; cool & dry skin
- occlusive therapy - polyethylene film to increase absorption of topical corticosteroids
- erosol - seldom used; no advantages
Categories:
- cleansing agents - detergents & solvents; isotonic saline
- protectants - powders; talc is better than cornstarch
- anti-infective agents - topical antibiotics, fungicides, etc.
- agents that relieve symptoms - analgesics; 0.5-3% camphor; 0.1-0.2% menthol; local anesthetics used with occlusive dressing
- anti-inflammatory agents - corticosteroids are most effective
- ntralesional injections - corticosteroid suspension (triamcinolone acetonide)
Dermatitis
Superficial skin inflammation, characterized histologically by epidermal edema and clinically by vesicles (acute), poorly marginated redness, edema, oozing, crusting, scaling, pruritis, and lichenification caused by scratching and rubbing.
Contact dermatitis
atopic dermatitis
herpes simplex dermatitis
herpes zoster dermatitis
dermatitis herpetiformis
pruritic dermatitis of vulva associated with extramammary Paget's disease
Bacterial Infections
Many bacteria normally inhabit the skin. It is important to realize this when looking at culture results. Infections may be primary or secondary. Primary infections are usually treated successfully with systemic antibiotics but, secondary infections are more difficult to treat with antibiotics and require more complicated treatment approaches. Recurrent infections indicate that an underlying systemic disorder is likely to be involved.
cellulitis of fifth digit
streptococcus pyogenes
plantar abcess and ascending cellulitis
necrotizing cellulitis
cutaneous folliculitis
erythrasma
impetigo (S. aureus)
Fungal Infections
Fungal infections invade the ded tissues of the skin or its appendages (stratum corneum, hair, nails). Yeast infections usually occur in moist, occluded areas of the skin, appendages of the skin, or mucous membranes.
ringworm
candida gram-stain from vagina secretions
candida in Pap smear
vaginal candida
Parasitic Infections
scabies
scabies mite
hookworm infection with ringworm (often misdiagnosed as scabies)
lice and nits
adult crab louse
adult body louse
adult head louse
Viral Infections
plantar warts
anogenital warts
genital warts in HIV+ patient
herpes simplex
Hair & Sebaceous Glands
acne
acne
Scaling Papular Diseases
Scaling papular diseases are either eczema or papulosquamous diseases which usually have sharp margins and lack signs of epitheliual disruption, such as wetness, crusts, fissures, and excoriations.
psoriasis
psoriasis
rosea
lichen planus
lichen planus
Inflammatory Reactions
erythema
erythema
Reactions to Sunlight
The skin may respond to excessive sunlight in several ways: sunburn, chronic changes, or photosensitivity.
Bullous Diseases
dermatitis herpetiformis
pemphigus
Cornification Disorders
parakeratotic columns (histological)
precancerous actinic keratosis (sunlight damage)
Pressure Sores
Pressure sores most often occur in patients with diminished or absent senstion or who are debilitated, emaciated, paralyzed, or long bedridden. Tissues over the sacrum, ischia, greater trochanters, external malleoli, and heels are especially susceptible; other sites may be involved depending on the patient's position. Pressure sores can also affect muscle and bone.
decubitis ulcer
Pigmentation Disorders
Hypopigmentation may take the form of vitiligo, albinism, and postinflammatory hypopigmentation. Hyperpigmentation results from increased melanin deposition in the skin. It may be caused by hormone changes like Addison's disease, pregnancy, or anovular pill use, or in some cases from iron or silver deposits.
Sweating Disorders
Lack of sweating may occur from blockage of sweat gland ducts and retention of sweat. Excessive perspiration is due to overactivity of the sweat glands.
Benign Tumors
benign mole
malignant mole
dysplasic nevi
angioma
hemangioma
keratoacanthoma
keratoacanthoma
Malignant Tumors
Skin cancers are usually curable. Most arise in sun-exposed areas of the skin. They may also develop from x-ray or radium burns, or from arsenic ingestion.
basal cell carcinoma
squamous cell carcinoma
melanoma
melanoma
Paget's disease of nipple
Karposi's sarcoma
oral Karposi's sarcoma
Miscellaneous
Gangrene secondary to Raynaud's disease
Gangrene due to Raynaud's disease
Review Questions:
1. Explain how arrangement of skin lesions is diagnostic.
2. What diagnostic approaches would you use for a viral skin infection?
3. What is the difference between a macule and a papule?
4. What is the difference between a vesicle and a pustule?
5. What is the difference between lichenification and atrophy?
6. What is the difference between a scab and scales?
7. What is the difference between erosion and ulcers?
8. What would you use to alleviate burning and itching of the skin?
9. Which preparation would you use for scalp problems?
10. What type of preparation would provide the strongest medication for topical application?